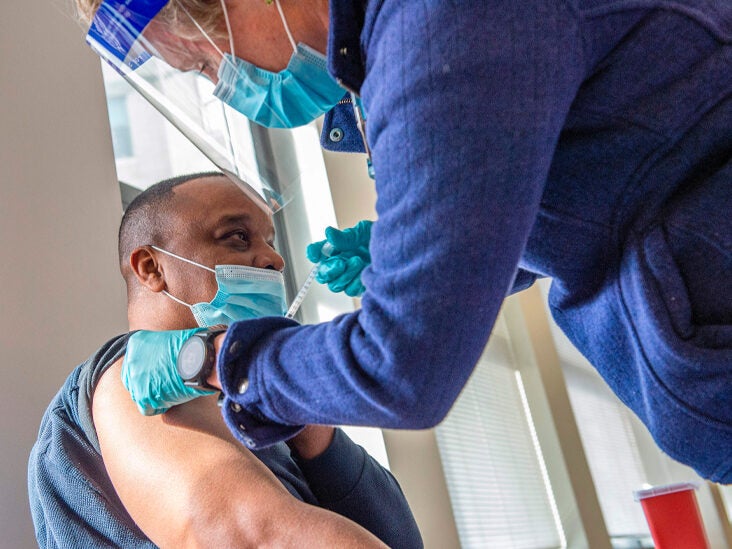
They are at a lower risk of reaction to the vaccine than someone with a history of allergic reaction to a vaccine or injectable medication. People with prior severe allergic reactions to foods, environmental allergens, venoms (insect stings), or oral medications are recommended to receive the COVID-19 vaccine. 
Following these five tips can make the decision easier. Making the decision about whether to get the vaccine can be difficult. 
Current Center for Disease Control (CDC) guidelines for people with a history of allergic reaction to vaccines or injectable medications is to consider a consultation with an Allergist/Immunologist prior to vaccination. When initial reports of reaction to COVID-19 vaccines came out, experts gathered to determine how to best counsel patients with a history of allergies regarding weighing the risk versus benefits of the vaccine. People with medication allergies or a history of allergic reactions are often wary of trying new medications or vaccines. Advanced Cardiac Life Support Classes For Medical Professionals.The Amber & Ben Patterson Wellness Walk.Designate Another Adult to Obtain Medical Care for Your Child.9 As the mRNA vaccines provide genetic information for the synthesis of SARS‐CoV‐2 spike protein, we postulate that a similar, albeit narrower range of autoantibodies may be induced. 7, 8 COVID‐19 infections were found to increase autoantibodies targeting a wide variety of tissues. Infections and vaccines can occasionally cause new‐onset or flare of autoimmune‐mediated diseases. Whilst it is possible that the dermatomyositis is coincidental to administration of the vaccine, the balance of probability given the temporal relationship and the severity of the symptoms following the first dose makes it difficult to recommend completing the vaccination regime. The patient did not receive the second dose in view of the adverse event after the first dose. 2, 3, 4 Whilst there have been reported cases of exacerbation of autoimmune disorders such as subacute cutaneous lupus erythematosus flare triggered by COVID‐19 vaccine, 5, 6 we describe, in this report, a novel case of dermatomyositis as an adverse reaction to mRNA COVID‐19 vaccine, with no prior history of connective tissue disorder. At last follow‐up, his prednisolone dose has been tapered to 10 mg per day.Ī spectrum of cutaneous reactions has been reported with both Moderna and Pfizer mRNA COVID‐19 vaccines, 1 with most skin biopsies showing a range of spongiotic and interface changes. Intravenous immunoglobulin infusion and hydroxychloroquine was subsequently added, resulting in resolution of symptoms and normalization of his serum muscle enzymes. The rashes and systemic symptoms improved after the treatment but worsened each time prednisolone was tapered below 20 mg per day. The patient was initially given topical corticosteroid and a tapering course of oral prednisolone. 
The patient declined muscle biopsy and further evaluation for malignancy. Chest radiograph had no features of interstitial lung disease. However, no immune deposits were noted on direct immunofluorescence. Dermal mucin was increased as highlighted by Alcian Blue stain (Figure 1D). Histopathological examination revealed epidermal atrophy, attenuation of the rete ridges and vacuolar interface changes, associated with sparse dermal inflammatory infiltrate composed of lymphocytes and no eosinophils (Figure 1C). Skin punch biopsy of a chest lesion was performed. Needle electromyography revealed spontaneous insertional activity with fibrillation potentials, positive sharp waves, and small polyphasic motor unit potentials in the proximal upper and lower limbs, suggestive of a myopathic disorder. An extended myositis antibody panel did not detect the presence of myositis‐specific or myositis‐associated antibodies. Anti‐extractable nuclear antigens antibody tests (Smith, ribonucleoprotein, Ro, La, Scl‐70, Jo‐1) were negative. Anti‐nuclear antibody test was positive with a titer of 1:160 (nucleolar staining pattern), but anti‐double‐stranded DNA antibody levels and serum complements (C3 and C4) were within normal range. Full blood count, urea and electrolyte levels, and thyroid‐stimulating hormone levels were unremarkable. Erythrocyte sedimentation rate was elevated at 56 mm/hr. Laboratory investigations showed raised muscle enzymes with serum aldolase levels of 6.8 U/L and alanine transaminase levels of 70 U/L. (D) Mucin, highlighted by special stain Alcian blue, is noted in the superficial dermis (C) Histology from the punch biopsy of the chest lesion shows epidermal atrophy, vacuolar interphase changes with sparse inflammatory infiltrate. (A) and (B) Erythematous rash with telangiectasis on chest and both medial cheeks sparing nasolabial folds.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
